How diverse is NC's obstetric delivery workforce?
By Julie Spero
Feb 5, 2020
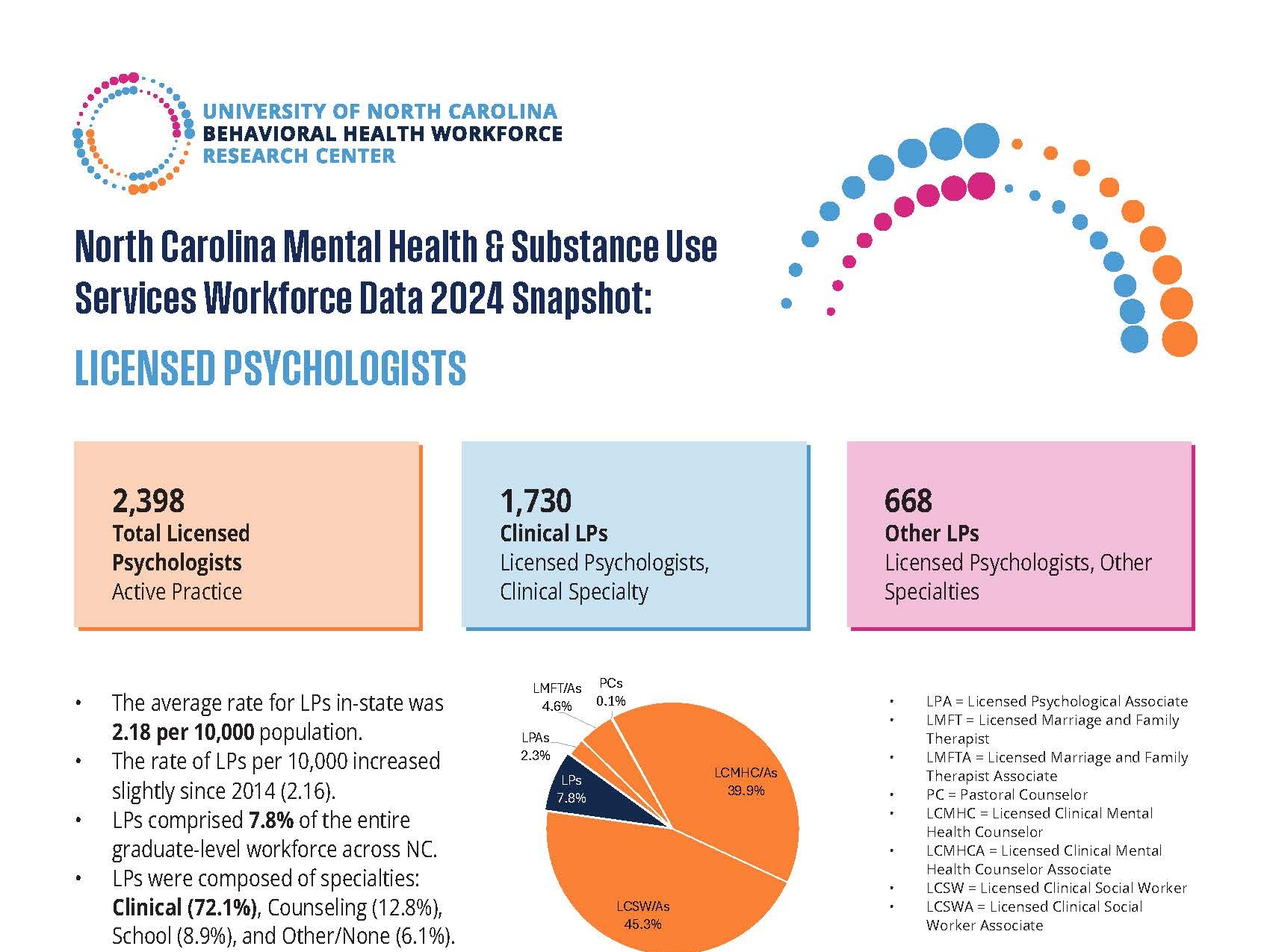
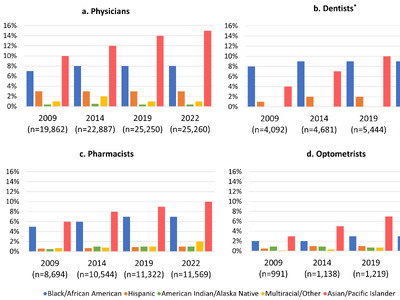
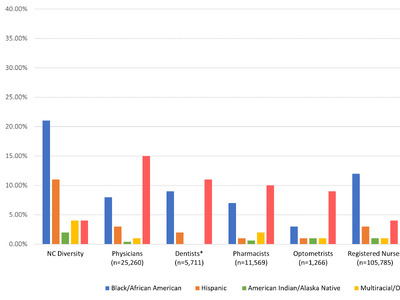
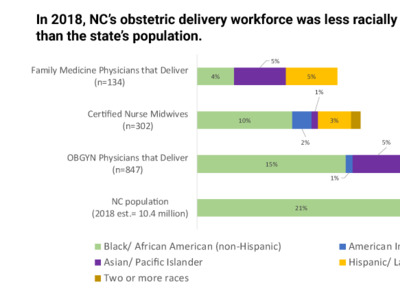
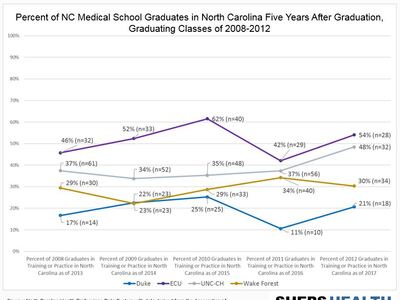
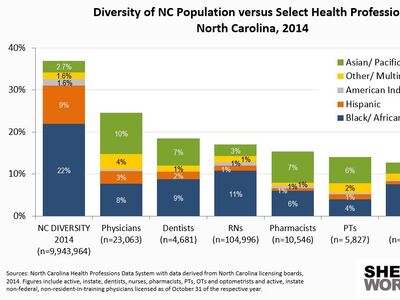
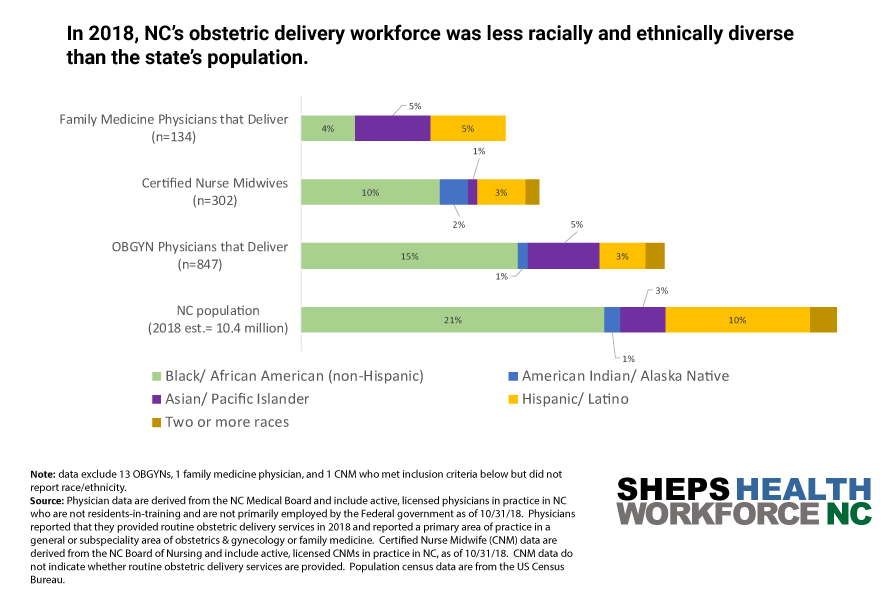
- In 2018, 21% of NC’s population identified as black or African American, compared to 13% of the state’s obstetric delivery providers.
- Similarly, 10% of NC’s population identified as Hispanic or Latino in 2018, compared to 3% of NC’s obstetric delivery providers.
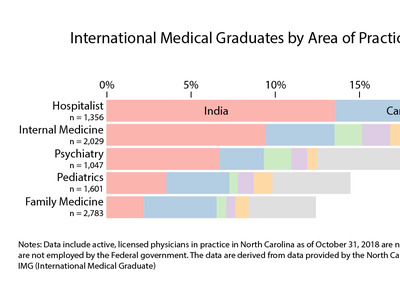
- Additionally, only five black family medicine physicians reported providing routine obstetric delivery services in 2018.
- In North Carolina, infant mortality rates are higher for non-Hispanic black babies than for non-Hispanic white babies, and this gap has persisted for nearly 20 years. [1] In 2018, black infants were almost two and a half times more likely to die than white infants. [2, 3]
- Relative to white patients, black patients report worse communication and lower shared decision-making with physicians. [4] Racial concordance, when patients and physicians identify as the same race, is associated with better patient-physician communication. Training can help improve communication between non-racially concordant providers and patients.
[1] Di Bona, V. Jones-Vessey K, Cobb SM. Running the numbers: disparities in infant mortality: examining perinatal periods of risk.NCMJ 2020; 81: 70-74.
[2] NC Department of Health and Human Services State Center for Health Statistics, 24 Sept 2019. 2018 NC Infant Mortality Report, Table 3b: Infant Mortality Racial Disparities Between White Non-Hispanics & African American Non-Hispanics: 2014-2018.Accessed 2/5/20 at: https://schs.dph.ncdhhs.gov/data/vital/ims/2018/table3b.html.
[3] Bonner L. Urban or rural, black lives in NC are being cut short almost before they begin.News & Observer, 1/29/20.Accessed 2/5/20 at: https://www.newsobserver.com/news/politics-government/article239388203.html
[4] Shen MJ, Peterson EB, Costas-Muniz R, Hernandez MH, Jewell ST, Matsoukas K, Bylund CL. The effects of race and racial concordance on patient-physician communication: a systematic review of the literature. J Racial Ethn Health Disparities, 2018; 5(1):117-140.